Our research: case studies
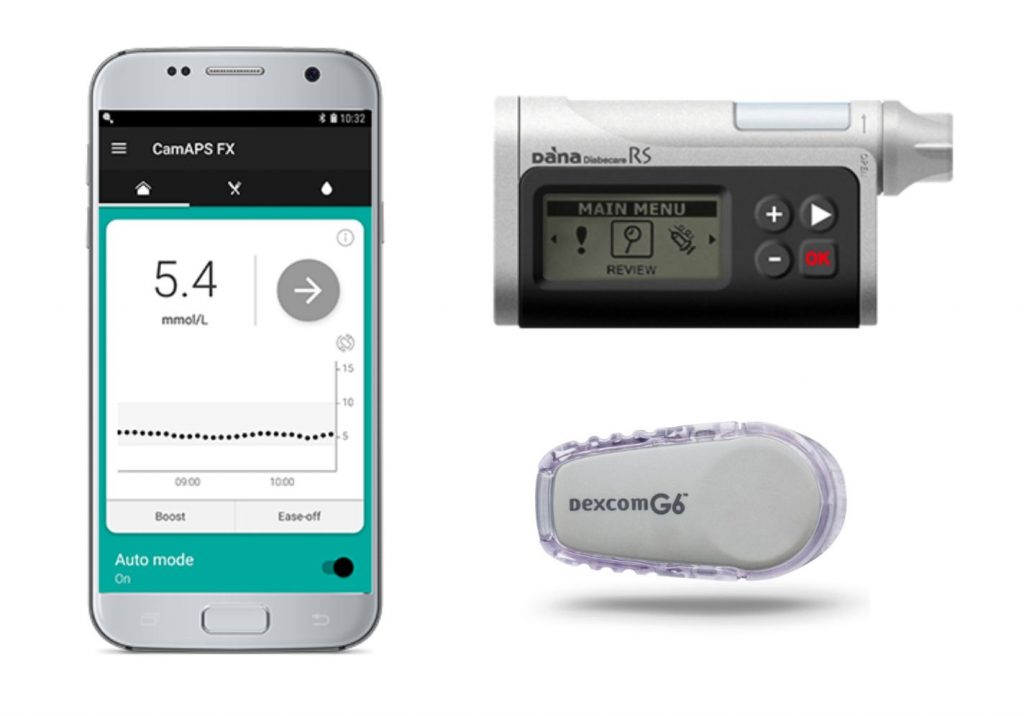
Artificial pancreas is helping protect very young children with type 1 diabetes
Researchers compared the performance of the artificial pancreas, which uses an algorithm to determine the amount of insulin administered by a device worn by the child, against ‘sensor-augmented pump therapy’.
Management of type 1 diabetes is challenging in very young children, because of a number of factors including the high variability in levels of insulin required and in how individual children respond to treatment, and their unpredictable eating and activity patterns.
To manage children’s glucose levels, doctors increasingly turn to devices that continuously monitor glucose levels and deliver insulin via a pump, which administers insulin through a cannula inserted into the skin. These devices have proved successful to an extent in older children, but not in very young children.
Professor Roman Hovorka, developed an app – CamAPS FX – which, combined with a glucose monitor and insulin pump, acts as an artificial pancreas, automatically adjusting the amount of insulin it delivers based on predicted or real-time glucose levels. It is a ‘hybrid closed loop system’, meaning that the child’s carer will have to administer insulin at mealtimes, but at all other times the algorithm works by itself.
The research team found the device performed better than current methods and parents found using this device life-changing. Read the full story from January 2022.

Brain receptor uses nutritional state to control growth and age at puberty
Researchers have discovered how a receptor in the brain, called MC3R, detects the nutritional state of the body and regulates the timing of puberty and rate of growth in children and increases in lean muscle mass.
It was previously thought growing taller and reaching sexual maturity may have been related to access to food for pregnant women and children, but researchers have now found it might be related to a receptor in the brain.
It is already known that signals reach the brain to indicate the body’s nutritional state. In a part of the brain called hypothalamus, hormones act on a small group of neurons that produce signals called melanocortins.
The melanocortins act on a variety of receptors, two of which are present in the brain. One of these, the melanocortin 4 receptor (MC4R) has previously been shown to regulate appetite and lack of MC4R results in obesity, but the MC4R system does not control the effect of nutrition on growth and timing of puberty.
Researchers found that in response to nutritional signals the MC3R system controls the release of key hormones regulating growth and sexual maturation, showing the brain can sense nutrients. This study could help people with the management in growth and puberty disorders.
Read the full press release from November 2021.

Artificial pancreas trialled for outpatients with type 2 diabetes for first time
An artificial pancreas could soon help people living with type 2 diabetes and who also require kidney dialysis.
Tests led by the University of Cambridge and Inselspital, University Hospital of Bern, Switzerland and supported by the NIHR Cambridge BRC, show that the device can help patients safely and effectively manage their blood sugar levels and reduce the risk of low blood sugar levels.
Diabetes is the most common cause of kidney failure, accounting for just under a third (30%) of cases. Kidney failure increases the risk of hypoglycaemia and hyperglycaemia – abnormally low or high levels of blood sugar respectively – which in turn can cause complications from dizziness to falls and even to coma.
Managing diabetes in patients with kidney failure is challenging for both patients and healthcare professionals. Many aspects of their care are poorly understood, including targets for blood sugar levels and treatments. Most oral diabetes medications are not recommended for these patients, so insulin injections are the most commonly used diabetes therapy – though optimal insulin dosing regimens are difficult to establish.
The researchers showed that the artificial pancreas – developed for patients with type 1 diabetes – can also be used to support patients living with both type 2 diabetes and kidney failure.
Unlike the artificial pancreas being used for type 1 diabetes, this version is a fully closed loop system – which means it can function entirely automatically. without any input from patients.
In the trial patients were split into two groups, one using the control treatment and the other using the artificial pancreas. Those using the artificial pancreas spent on average 53% of their time in the target blood sugar range, compared to 38% when they used the control treatment. The length of time they had potentially low blood sugar levels, or ‘hypos’, was also lower.
Nine out of ten (92%) reported that they spent less time managing their diabetes with the artificial pancreas than during the control period, and similar numbers (87%) were less worried about their blood sugar levels when using it.
This is an abridged version of the press release which was first published on our website on August 5, 2021.

A single gene could be the reason why some of us carry an extra 30 pounds of fat
New research has found that one in every 340 people might carry a mutation in a single gene that makes them more likely to have a greater weight from early childhood.
By the time they reach adulthood, they could be up to 30 pounds (13.6 kg) heavier with the excess weight likely to be mostly fat.
The NIHR Cambridge BRC-supported study found that when the MC4R gene does not work properly, our brains think we have lower fat stores than we do, signalling that we are starving and need to eat.
These results were found by studying the MC4R gene in a random sample of around 6,000 participants born in Bristol in 1990-91, who were recruited to Children of the 90s, a health study based at the University of Bristol.
Based on the frequency of mutations in this study, it is possible that around 200,000 people in the UK could carry a substantial amount of additional fat because of mutations in MC4R.
In the longer term, knowledge of the brain pathways controlled by MC4R should help in the design of drugs that bypass the signalling blockade and help restore people to a healthy weight.
This is an abridged version of the article first published on our website on 28 May 2021.

How do our genes affect our weight
Researchers have known for some time that body weight is strongly influenced by genetics, though the exact genes that influenced weight gain remained elusive.
Researchers in Cambridge have discovered genetic variants (small changes in DNA) that help protect people from obesity, type 2 diabetes and heart disease. These findings could help researchers to develop drugs for people who have weight problems.
Obesity is a serious problem; it can lead to heart disease, type 2 diabetes, stroke and mobility problems.
Cambridge researchers studied a gene called ‘MC4R’ which is known to regulate weight by acting like an ‘off’ switch for appetite. By looking at samples from half a million volunteers in the UK, they found that in naturally lean people small changes in the MC4R gene were able to limit their appetite to prevent weight gain. They also found that some people had a version of the gene that defended against the risk of diseases associated with obesity such as type 2 diabetes and heart disease.
These findings help explain the genetics of why slim people have an advantage when managing their weight. The research could now help researchers to develop new treatments to help people reduce excess weight.

Artificial pancreas an international success
Poor management of blood sugar levels for people with diabetes can lead to serious health complications such as kidney disease, heart disease or eyesight problems.
Cambridge researchers from the Metabolic, Endocrinology and Bone research theme collaborated with our Women’s Health and Paediatrics theme to develop a world-leading artificial pancreas system (a continuous glucose monitoring device) for people with type 1 diabetes. The system uses smartphone technology to communicate with an insulin pump and a continuous glucose monitor.
The system calculates and delivers the correct amount of insulin needed at any particular time, therefore cutting out the need for injections, improving glucose control and reducing the risk of hypoglycaemia (low blood sugar). The continuous glucose monitor is worn 24/7 meaning that blood sugar levels are continuously measured including through the night leading to less disturbed sleep patterns.
More than 150 children and adults have trialled the device and compared it with the best available therapy in diabetes clinics internationally, including the UK, Germany and Austria. Longer-term trials are ongoing, testing the artificial pancreas in newly diagnosed children and adolescents and young children aged 1 to 7 years old.

